Peripheral neuropathy was long known to be a nerve disease that causes symptoms like tingling, burning, and pain in feet and hands. While those are the most common and often first felt, in actuality, those symptoms of neuropathy are now just thought to be the tip of the iceberg.
Seemingly unrelated symptoms are also traced back to neuropathy because any function that involves peripheral nerves can be affected by peripheral nerve damage.
The peripheral nerves are all of the nerves outside of the brain and spinal cord. Therefore anything outside of the brain and spinal cord can be affected by peripheral neuropathy. And that’s a lot.
Learning about the varying types of neuropathy symptoms can help you better understand your condition.
Types of Peripheral Nerves
The type of neuropathy symptoms you develop largely depends on the type of nerve fiber that has been damaged.
Damage to one nerve type is most common, but damage can be done to any number of nerve types at the same time.
The more nerve types that are affected, the more variety of symptoms will be felt.
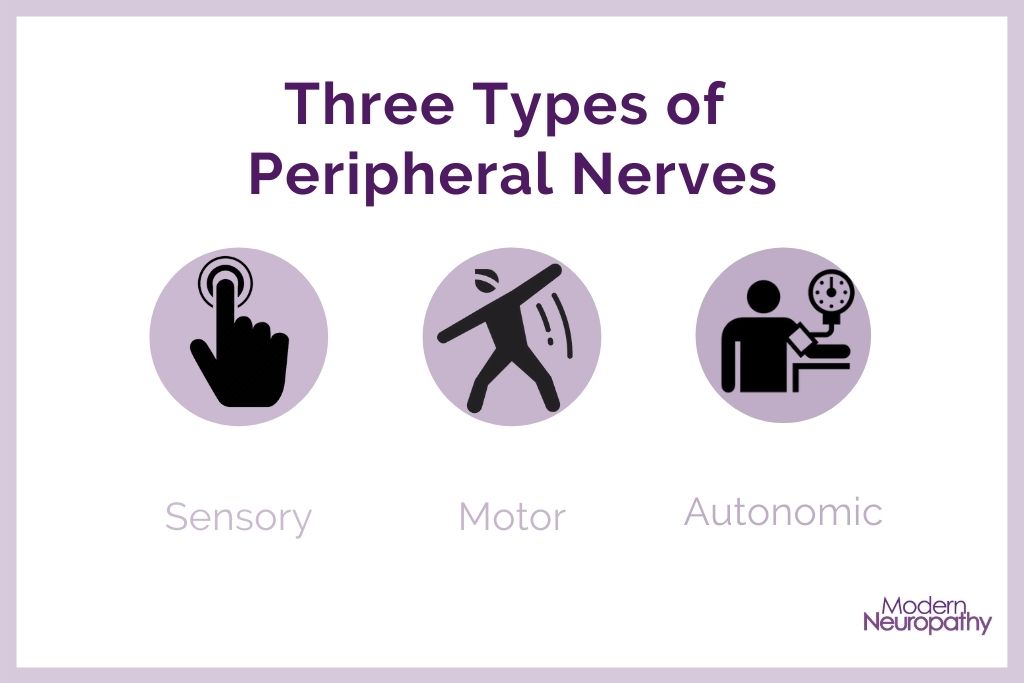
Peripheral nerve fibers can be broken down into three types:
- Sensory: sensations and sensory input, like touch, sight, and smell
- Motor: movement and reflex, like walking and balance
- Autonomic: automatic body function, like blood pressure, digestion, and temperature regulation
Next, you will learn about what symptoms each one of these nerve fiber types may cause so you can better identify what is going on with your own body if you are having symptoms of neuropathy.
Sensory Nerve Damage Symptoms

Symptoms of damage to sensory nerves are typically the first felt, as your sensory nerves are the thinnest and the most vulnerable to damage.
Because sensory nerve damage directly affects your body’s sensory information, they can be the most bothersome.
The majority of people with sensory damage first feel symptoms in the feet that then progress upwards. But sensory symptoms can start anywhere on the body. (1)
When sensory nerves become damaged, their behavior can become unpredictable, causing inappropriate or incorrect signaling.
These confused messages go to the brain, but the brain doesn’t know how to interpret them. So the brain then responds with sensations it knows.
Sensory nerve damage symptoms typically take on one or several types of symptoms.
Common types of sensory symptoms include:
- Paresthesia: painless abnormal sensations
- Dysesthesia: abnormal sensations that may be severe enough to be considered painful
- Allodynia: hypersensitivity to light touch that is barely noticeable to others
- Hyperalgesia: extreme sensitivity to what is only slightly painful to others
- Hypoesthesia: unusually low sensation to temperature
- Anaesthesia: loss of feeling
Next is a more in-depth look at each type of sensory symptom.
Paraesthesia Symptoms
Paresthesia symptoms of neuropathy are usually painless sensations that are not normal. Though they are not considered to be painful, they are often still very uncomfortable. These include bizarre, phantom, or unusual feelings that are often hard to even describe.
To make paresthesia symptoms even more confusing, they don’t necessarily stick to a localized area and can pop up to any part of the body stimulated by sensory nerves. Mouth, scalp, face, genitals…anywhere.
Paresthesia symptoms are very common to sensory symptoms of neuropathy and are the kind that are often worse at night.
Examples of paraesthesia symptoms are these sensations, or similar:
- Tingling
- Itching
- Pins and needles
- Numbness, but not actually numb
- Buzzing
- Vibrations
- Tickling
- Crawling skin
- Wetness or dripping water
- Walking on marbles
- Stocking or glove sensation
Dysesthesia
Dysesthesia symptoms of neuropathy are similar to paresthesia, but more severe and may be painful, even without apparent cause for pain.
Examples of dysesthesia symptoms are these sensations, or similar:
- Mild to severe pain
- Burning or stinging
- Stabbing
- Ice cold
- Electrical shock-like
- Aching
- Throbbing
- Heat sensitivity
- Cold sensitivity
- Severe itching
Allodynia
Allodynia symptoms can be described as a hypersensitivity to light touch that would be barely noticeable to others. Something as normal as clothes, socks, or bedsheets triggers a reaction, often felt as pain. But could also be described as usual sensations, like sandpaper or needles.
Hyperalgesia
Hyperalgesia symptoms are similar to allodynia symptoms but with a slight difference. These symptoms are also described as an extreme sensitivity, but rather than sensitivity to what others feel is normal, these symptoms are an extreme sensitivity to what others would think is only slightly painful.
Examples of hyperalgesia symptoms are these sensations, or similar:
- Extreme sensitivity to heat or cold
- Excessive pain with exercise
Hypoesthesia
Hypoesthesia symptoms are those that have an unusually low sensation to heat or cold. Described as a loss of ability to feel temperature, these symptoms can be dangerous when exposed to things like extreme weather, water temperatures, or cooking.
Anesthesia
Anesthesia symptoms are those that result in a loss of feeling and can lead to loss of balance and difficulty walking. Loss of feeling also presents a danger of infection when cuts and infections go unnoticed. When anesthesia symptoms combine with other types, like pain, that’s when you get symptoms that especially make no sense, like pain and numbness all at the same time.
Motor Nerve Damage Symptoms

Because motor nerves are larger in size than sensory nerves, they are relatively sturdier. Also, they are protected by a fatty protective covering, called myelin sheath. With their size and protection, they are more resilient and tend to not become damaged as quickly as sensory nerves.
Therefore, motor neuropathy symptoms tend to appear after symptoms of sensory nerve damage.
When motor nerves become damaged, they let you know with symptoms that are very different from those of the sensory nerves.
As the nerves that innervate your muscles begin to die out, they also stop being able to send impulses properly. This might mean that the impulse isn’t as strong, or it could mean that the impulse isn’t coming through altogether.
If enough neurons fail to send their impulses, the signal coming into that particular muscle can be weakened, meaning you can’t pick up that glass of water quite as well as you used to be able to.
Over time, this weakened impulse leads to muscle atrophy, which is a weakening or even shrinkage of the muscle tissue.
Depending on where this happens in the body, the consequences can be varied, including:
- Increased risk for falls
- Difficulty driving
- Difficulty walking
- Loss of balance
The muscles in your legs aren’t only responsible for helping stand and get around. They also do the very important work of helping to make sure that gravity doesn’t cause all of your blood to pool in the lower parts of your body. When the neurons innervating these muscles start to fail, your muscles aren’t able to do this work as effectively.
As blood collects in the lower parts of your body (known as edema), your legs will:
- Swell
- Feel tightened
- Feel stiff
- Feel heavy
As dying neurons fire off spontaneous high-frequency discharges in later stages, you may feel:
- Twitching
- Cramping
Other signs of motor neuron damage can include:
- Tremors
- Restless legs syndrome
- Abnormal feelings in muscles
- Foot deformation, in advanced stages
Autonomic Nerve Damage Symptoms
The autonomic nerves are those that carry messages from your brain and spinal cord out to your internal organs. (2) Together, they control functions that happen automatically, like:
- Blood pressure
- Heart rate and breathing rate
- Body temperature
- Digestion
- Metabolism
- Fluid production in glands
- Detoxification
- Sexual response
Autonomic nerve damage is among the least common, therefore autonomic symptoms are those that are experienced less frequently.
However, they can be among the most serious given that your autonomic nervous system controls many of your vital functions.
Some of the more common symptoms of autonomic nerve damage include: (3, 4, 5)
Cardiovascular
- Dizziness when standing
- High blood pressure
- Low blood pressure
- Rapid heart rate at rest
- Irregular heartbeat
Digestion
- Diarrhea
- Constipation
- Bloating
- Belching
- Nausea
- Vomiting
- Difficulty swallowing
- Heartburn
- Loss of appetite
Body Temperature
- Loss of bladder control
- Difficulty sensing a full bladder
- Inability to fully empty bladder, which can lead to urinary tract infections
- Difficulty starting urination
Blood Sugar
- Loss of ability to detect hypoglycemia (low blood glucose)
Sexual
- Men: erectile dysfunction
- Women: dryness, low libido
Progression of Neuropathy Symptoms
Symptoms of neuropathy can start rapidly (acute) or develop and progress slowly over time (chronic).
The location where neuropathy symptoms start depends on the cause of nerve damage.
For instance, in the case of a compressed spinal nerve, symptoms may develop at the location of the compression or anywhere along the length of the nerve and are usually felt more on one side of the body.
In the case of systemic causes of peripheral neuropathy, like diabetes or toxicity, symptoms are more commonly felt first in the feet. Which then gradually spreads up the legs toward the center of the body as damage progresses.
Summary
Symptoms of neuropathy can be widely different from one person to the next, depending on the location and type of nerve that is damaged.
Sensory, motor, and autonomic nerves have symptoms that differ from one another.
Understanding what symptoms of nerve damage mean can help reduce the confusion that is often felt by those suffering from neuropathy.
Is Undetected Kidney Disease Causing You Uremic Neuropathy?
A shocking 30 million people in the United States are dealing with kidney disease, and…
Complete Guide to CBD for Neuropathy

CBD seems to be in everything these days — oils, lotions, drinks, gummies, sprays, supplements,…
These 7 Foods Improve Nerve Health, Here’s Why

The foods we choose have a surprisingly direct impact on the health of the nervous…
4 Clean CBD Brands You Can Trust

CBD has grown in popularity over recent years, especially for anxiety, pain, and sleep disorders.…
8 Best Supplements for Neuropathy
We know that nutritional supplements -- in addition to a healthy diet -- can help…
What is Peripheral Neuropathy?

If you already have it, you basically know what peripheral neuropathy is. It just refers…
What Does My Peripheral Neuropathy Diagnosis Mean?

It’s a mouthful. Confused by what it even means? If you have a peripheral neuropathy…
Best Value Red Light Therapy Panel Goes to Mito

As the popularity of red light therapy has grown quickly over the past few years,…












